Table of Contents
Glycopyrrolate and oxybutynin belong to a class of medications known as anticholinergic drugs, which are often used to treat excessive sweating, or hyperhidrosis. In a general sense, anticholinergic medications block the neurotransmitter acetylcholine within the peripheral and central nervous systems. Essentially, this means that they impede the ability of the sympathetic nerves to communicate with the body’s sweat glands and prevent them from producing sweat.
Pros and Cons of Glycopyrrolate and Oxybutynin
Before starting a course of either medication, you should carefully consider the pros and cons of each. While these medications can be effective, be aware that there are also many negative side effects. Oral medications are typically prescribed when other treatments have failed to show significant positive results. Though no oral medications are currently FDA-approved specifically for the treatment of hyperhidrosis, several have a long history of off-label use for that specific purpose.
Pros of Glycopyrrolate and Oxybutynin
- Available in a convenient pill form.
- Oxybutynin is also available as a topical gel and as a transdermal patch.
- Ability to scale dosage – this allows you to experiment to find the right dose that’s effective for stopping excessive sweating while leading to the fewest side effects.
- Oxybutynin is relatively inexpensive medications, accessible for a wide variety of people.
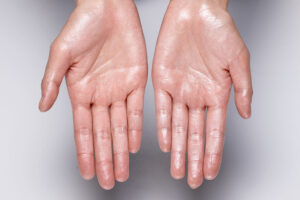
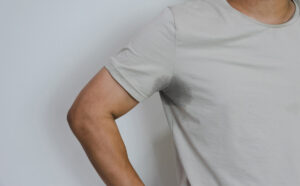
- Effective in preventing plantar (foot), palmar (hand) and axillary (armpit) hyperhidrosis. In fact, one study reports that 70 percent of patients saw decreased sweating symptoms related to axillary and palmar hyperhidrosis, while 90 percent reported improvement in plantar hyperhidrosis symptoms.
Cons of Glycopyrrolate and Oxybutynin
- Drowsiness
- Blurred vision
- Fast, weak pulse or increased heart rate
- Irregular heartbeat
- Fever
- Increased blood pressure
- Fast, shallow breathing
- Dry mouth
- Loss of taste
- Headache
- Confusion
- Fainting
- Difficulty falling or staying asleep
- Nausea
- Vomiting
- Dry eye
- Nasal congestion
- Decreased mental alertness
- Bloating
- Constipation
- Dizziness
- Eye pain
- Anxiety
- Irritability
- Flushing or redness in the face and skin
- Constipation or urinary retention
- Hallucinations
Oral medications are usually most effective when used as adjunctive therapy with other treatment options, like topical medicines and antiperspirants, in order to decrease hyperhidrosis symptoms. People who usually find the most success with oral hyperhidrosis medications are those who experience excessive sweating all over the body.
Before prescribing an oral medication, your physician may encourage you to try other remedies, such as Botox injections, local permanent treatment options, or topical creams. Oral medications, however, can be especially helpful when the cause of excessive sweating is identified, but cannot be eliminated or remedied – for example, if an existing medication regimen causes excessive sweating but cannot be changed or abandoned without causing bigger issues.
What You Need to Know About Each Medication
While not specifically developed to treat hyperhidrosis, anticholinergic drugs like glycopyrrolate and oxybutynin are often prescribed for this purpose. This class of drug binds with acetylcholine, thus preventing it from being used throughout the body. Receptors are located throughout the autonomic nervous system and expand through the whole body – resulting in a system-wide, rather than localized, effect.
Here’s the kicker: These medications also block receptors completely unrelated to the sweat glands and perspiration, which can lead to unintended and unwanted side effects. Let’s take a closer look at what you need to know about each of these oral medications.
Glycopyrrolate
Glycopyrrolate is the most commonly prescribed anticholinergic for excessive sweating. It’s primarily prescribed to treat ulcers and gastric secretions in adults and drooling in children, since it decreases stomach acid and saliva production. In addition, it reduces the body’s ability to sweat. Glycopyrrolate in oral form is the most commonly prescribed anticholinergic drug for hyperhidrosis treatment – mainly because it causes fewer central nervous system side effects. People typically take glycopyrrolate as tablets or a liquid, by mouth, either two or three times per day on an empty stomach – usually one hour before or two hours after a meal. Appropriate dosage is based on your specific medical condition, documented response to treatment and body weight.
Before beginning a glycopyrrolate dose, your doctor will ask if you have ever had any of the following: glaucoma, difficulty urinating, enlargement of the prostate, ulcerative colitis, high blood pressure, overactive thyroid, coronary artery disease, disorders of the nervous system, or kidney or liver disease. In addition, you should notify your physician if you are pregnant, think you might become pregnant, or are currently breastfeeding.
To reduce the incidence of possible glycopyrrolate side effects, your physician may recommend that you begin taking it at a relatively low dosage and gradually increase as your body acclimates to the new medication. You should not increase the dosage or frequency of glycopyrrolate without consulting your doctor – doing so won’t improve your hyperhidrosis, but it will increase your chances of suffering adverse events and side effects.
The glycopyrrolate drug class has shown a high rate of effectiveness when studied – for example, one clinical trial has reported that up to 90 percent of patients taking glycopyrrolate saw a reduction in hyperhidrosis symptoms. Unfortunately, up to one third had to abandon therapy because of adverse side effects, which have been reported by up to 80 percent of participants taking these oral medications as part of clinical studies.
Glycopyrrolate can negatively interact with a wide variety of other medications, so make sure to tell your doctor about any prescription, over-the-counter or holistic medications you are currently taking before starting a round of glycopyrrolate. Depending on the potential combinations, your physician may choose to either change your dosage or monitor you carefully for side effects.
Glycopyrrolate dose helps reduce sweating by systematically reducing all body secretions, which can result in some annoying and uncomfortable side effects. For many people, glycopyrrolate side effects show up as minor irritations that can be mitigated through measures like drinking more water (which may increase urinary frequency), eating mints, or using eye drops. However, these side effects persist over time or grow worse, you should contact your doctor immediately.
While rare, the following side effects of glycopyrrolate can also occur and are especially dangerous. You should consult your doctor immediately if you experience any of the following:
- Urination problems: difficulty urinating or inability to urinate
- Hives
- Rash
- Diarrhea
- Difficulty breathing or swallowing
Anticholinergics are systemic medications, which means they cannot target any one particular area on the body in which sweating is most profuse; instead, they decrease sweating over the entire surface of the body, no matter whether that’s needed. If you’re not careful, this overall reduction in the body’s ability to cool itself through sweating can put you at risk of overheating. In essence, the sweating mechanism is turned off, which dramatically decreases the body’s ability to regulate its temperature.
Athletes and those who work outdoors should be especially careful when they take anticholinergics – and for these reasons, these types of patients may be considered ineligible for use of oral medication for the treatment of excessive sweating. The same is true for people who have a natural tendency to overheat. Taking these medications can dramatically hinder the body’s ability to cool itself down, leading to a dangerous situation.
In addition, the high cost of glycopyrrolate for sweating is a limiting factor for some people.
Oxybutynin
Oxybutynin chloride is often prescribed with elderly patients to treat urinary incontinence, overactive bladder or frequent urination. It is the second most commonly used anticholinergic drug to treat hyperhidrosis. Ideally, the lowest possible dose of oxybutynin should be used in order to minimize the risk of adverse side effects.
Oxybutynin tablets are often prescribed – both immediate and extended-release – as well as oxybutynin gel, oxybutynin syrup, or even an oxybutynin transdermal patch. No matter its form, oxybutynin is recommended to take with water on an empty stomach, though some physicians insist that patients with incontinence take the medication with food or milk in order to decrease the chances of an upset stomach. If your oxybutynin is prescribed as a time-release oral medication, be sure to follow the directions carefully. Swallow the tablet whole – do not crush, break or chew it, as doing so will adjust the time-release formulation. Drink lots of water or any other liquid of your choice. Also, be sure to take your oxybutynin tablet at the same time each day.
Oxybutynin dosage will vary from patient to patient, but usually hovers around 5 or 10 mg taken two or three times per day for adults and children over 12. The dosage rarely exceeds 30 mg per day. It is very important to use oxybutynin medication only as directed – no more, no less. Refrain from operating motor vehicles or other large machinery until you have an idea of how your body tolerates the oxybutynin drug.
One important consideration is that oxybutynin effects can cause a serious allergic reaction known as angioedema, which is life-threatening and requires immediate medical care. If you experience any of the following adverse reactions after taking oxybutynin, call your doctor or emergency medical care immediately: chest tightness or trouble breathing, body rash, itching, intense swelling of the face (including lips, throat, tongue, eyelids), hands, legs, feet or genitals.
Oxybutynin has been known to cause a negative reaction when combined with the following drugs and compounds: potassium, glycopyrrolate, donepezil, bupropion, tiotropium, secretin human, glycopyrronium tosylate, rivastigmine, ketoconazole, and galantamine. Tell your physician if you are taking any of these medications. Your doctor may choose to either change your dose of oxybutynin, watch you carefully for side effects of oxybutynin, or modify other medications you take while you are taking oxybutynin.
Certain pre-existing medical conditions can affect your body’s acclimation to oxybutynin, especially with elderly patients. Any of the following conditions have the potential to react negatively with oxybutynin: dementia, overactive thyroid, enlarged prostate, heart disease, hypertension, intestinal or stomach problems, Parkinson’s disease, toxemia of pregnancy, urinary bladder blockage, or glaucoma. Make sure to tell your doctor if you are currently suffering from any of these conditions.
Patients are more likely to see anticholinergic side effects right after beginning a course of oxybutynin or after an increase in dosage. Any of these symptoms should be reported to a physician as soon as possible – your doctor can help you determine whether your side effects are severe enough to need medical attention or if they will likely go away as your body acclimates to the new medication.
In addition, oxybutynin and alcohol are a dangerous combination; oxybutynin exacerbates the effects of alcohol and other CNS depressants like antihistamines, tranquilizers, sedatives, muscle relaxers, and some prescription pain medications.
New Topical Applications Available
One of the biggest drawbacks to any oral medication for the treatment of hyperhidrosis is its systemic nature – it can’t be localized, and it often creates side effects that affect the entire body. However, new treatment options featuring glycopyrrolate and oxybutynin are now being developed and marketed that are topical in nature, which allow patients to concentrate treatment within a particular, localized problem area.
While topical creams containing glycopyrrolate and oxybutynin are now available, their efficacy is still under review. Some early indications show that the creams may have trouble penetrating the outer skin barrier. In addition to topical creams, a new product called Qbrexza features glycopyrronium tosylate within a medicated wipe that can be used to topically treat hyperhidrosis. It is typically used once per day to prevent excessive sweating.
In addition, there is some indication that topical treatments like Qbrexza can be used in conjunction with iontophoresis treatments, which use low-level electrical currents to push medications – usually anticholinergics – through the skin of a particular body area submerged in water. These treatments have shown best results when treating excessive sweating of the hands and feet.
Future Studies and Uses
While no cure is yet available, treatments for hyperhidrosis continue to improve. Excessive sweating affects 3 to 5 percent of the world’s population, and medical experts are still trying to understand the causes of hyperhidrosis. Many current treatments, including the use of anticholinergics, can be invasive and ineffective. However, as this condition is further studied, researchers will be able to develop targeted and more effective treatments.
There is a great deal of promising research on the horizon for those who suffer from hyperhidrosis. Emerging treatments and technologies have great potential to make a profound difference in quality of life. For example, topical medications have great promise in treating hyperhidrosis without many of the negative anticholinergic effects experienced when taken orally. The theory is that being able to apply a topical anticholinergic to a local area will stop or dramatically reduce sweating in that area without the drawbacks associated with an oral dose, which affects the entire body.
Many studies and intended future use of both glycopyrrolate and oxybutynin are on the horizon. One of the most encouraging is the planned use of glycopyrrolate in a topical cream that would be used to directly target the eccrine glands – it would likely include a 1 percent or 2 percent glycopyrrolate suspension. Oxybutynin also is currently being studied in connection with topical applications that would be more effective than current options. In preliminary studies, glycopyrrolate has shown promising results in the higher 2 percent suspension with very few side effects. Other studies have specifically explored a 2 percent glycopyrrolate pad, finding that some participants reported sweat reduction of up to roughly 62 percent. While existing studies have been small, a series of larger, double-blind studies could help further understanding of topical products’ potential to improve quality of life for people with excessive sweating.
In addition, while Qbrexza currently is indicated only for underarm use, additional research could have implications for additional hyperhidrosis treatment throughout the body.
Other Research and Product Possibilities
Along with various topical formulations, researchers are currently working to develop next-generation, non-injection Botox treatments for addressing plantar (foot), axillary (underarm) and palmar (hand) hyperhidrosis. In addition, the FDA-approved MiraDry is a medical device indicated for the treatment of underarm hyperhidrosis. This treatment involves heating the skin to the point that sweat glands are destroyed. Several other devices also are under development that employ various methods for heating the skin to destroy sweat glands.
Another new technology is fractional microneedle radiofrequency treatment, which sends energy into the reticular dermis – the lowest layer of the skin – without harming the epidermis, or the skin’s outer layer. FMR has been widely used to treat wrinkles and acne scars, and early studies show that it has potential to address hyperhidrosis as well. Early results indicate that many people undergoing treatment show significant improvement as soon as two months.
Lasers may also offer some benefit in the future for hyperhidrosis sufferers. Specifically, the 1064-nm Nd-YAG laser has potential, particularly when tested against underarm hyperhidrosis. In some studies, as many as 70 percent of participants showed improvement in self-reported assessments, while physicians’ assessments revealed upwards of 80 percent of participants showing improvement. With further study and refinement, this kind of therapy could be especially effective.
Additionally, ultrasound, which focuses ultrasonic energy within a localized area, is a new focus of interest and further study. In particular, the VASER ultrasound has been shown to improve symptoms for up to six months, but no data for longer time periods is currently available. Early results are encouraging, though more research and study are needed to determine exactly how effective various ultrasound methods may be in treating hyperhidrosis symptoms.
Treating Hyperhidrosis
Today, no cure for hyperhidrosis exists, but further research, medical knowledge, and understanding may expand to the point where a cure is within reach. Above all, scientists must understand the physiology of hyperhidrosis and how various drugs impact that physiology. Doing so can help lead to better therapies that are more effective with fewer side effects. Because hyperhidrosis is at least partly hereditary, understanding its underlying genetic sequence may also reveal additional clues for how best to prevent, treat, or cure the condition. Thankfully, as hyperhidrosis continues to garner awareness and attention, more researchers and medical professionals can get behind exploring new ways to improve quality of life for those with the condition.
If you sweat excessively and haven’t been able to find a treatment that works, the next logical step is to visit with your doctor. At this point, the physician may prescribe oral anticholinergic medicines to decrease the overall amount of sweat produced by your body. Glycopyrrolate and oxybutynin are the two most commonly used anticholinergic agents to treat hyperhidrosis.
Overall, medicines like glycopyrrolate and oxybutynin can be effective components of a comprehensive treatment plan for people with hyperhidrosis, though be prepared for negative side effects. If you’ve been prescribed one of these drugs, the information in this post can help you better understand how each medication works and what to expect in terms of potential side effects. And, as always, make sure you are working closely with your physician to manage your hyperhidrosis symptoms. Your doctor can help you further understand the full pros and cons of using systemic anticholinergic drugs for your specific situation.
You might also like...

Why Do I Sweat So Much? And So Easily?
WHY DO I SWEAT SO MUCH? : ARTICLE CONTENTS Sweating a lot? … when you workout, sleep, after eating, or

Is There a Hyperhidrosis Cure? 11 Hyperhidrosis Treatment Options
If you’re one of the roughly 8 million Americans who deal with excessive sweating (also known as hyperhidrosis), this article

How to Stop Sweating So Much? 9 Tips to Beat Unwanted Sweat
If you’ve ever suffered through an awkward sweaty hug, a slippery handshake, or a sweat-soaked job interview — this article